Are you or a loved one dealing with Parkinson’s disease and wondering if fasting could offer some relief? You’re not alone.
Many people are curious about how therapeutic fasting might impact Parkinson’s symptoms and overall brain health. Could something as simple as adjusting when you eat help protect your nerves or even support recovery? Experts are exploring how fasting triggers natural processes in your body that may reduce inflammation, promote nerve repair, and boost brain function.
You’ll discover what current research says about fasting and Parkinson’s disease, what benefits you might expect, and important safety tips before trying it yourself. Keep reading to learn how fasting could become a powerful tool in managing Parkinson’s and improving your quality of life.
Fasting And Parkinson’s Disease
Fasting has gained attention as a possible way to support brain health in Parkinson’s disease. This neurodegenerative disorder affects movement and muscle control. Research suggests fasting might slow disease progression and ease some symptoms. Scientists study how fasting influences brain cells and inflammation, which are key in Parkinson’s.
Fasting may activate processes that clear damaged cells and protect nerve tissues. These effects could help reduce the impact of Parkinson’s on the nervous system. Understanding different dietary methods offers insight into managing this condition better.
Dietary Approaches To Parkinson’s
Many diets aim to support brain function in Parkinson’s patients. Mediterranean and ketogenic diets are popular for their focus on healthy fats and antioxidants. These nutrients may reduce inflammation and oxidative stress in the brain.
Fasting is another approach gaining interest. It encourages the body to enter a state that promotes cell repair and reduces harmful molecules. Balanced nutrition remains essential to prevent nutrient deficiencies during fasting.
Fasting Types Explored
Intermittent fasting involves cycling between eating and fasting periods. Common patterns include 16 hours fasting with an 8-hour eating window. This method may improve brain cell health and reduce inflammation.
Time-restricted feeding limits food intake to certain hours daily. Prolonged fasting lasts longer than 24 hours and is less common for Parkinson’s patients. Fasting-mimicking diets offer reduced calories while maintaining nutrients. Each type impacts the body differently and requires careful planning.

Credit: www.maxhealthcare.in
Cellular Effects Of Fasting
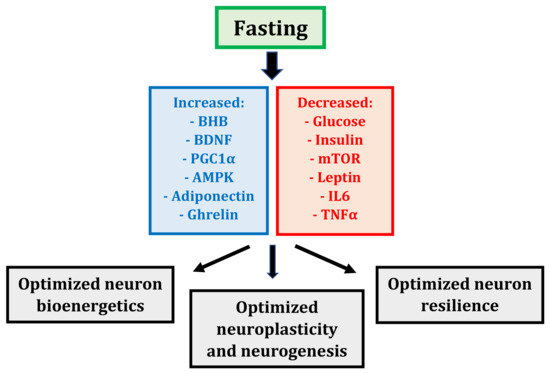
Fasting influences many processes inside our cells. These changes may support brain health and help manage Parkinson’s disease symptoms. At the cellular level, fasting triggers important effects that promote cell repair and improve brain function. Understanding these effects sheds light on how fasting could benefit people with Parkinson’s.
Autophagy Activation
Autophagy is the body’s way to clean out damaged cells. It breaks down old parts and recycles them to build new ones. Fasting activates autophagy, which helps clear harmful proteins linked to Parkinson’s disease.
This cellular cleanup reduces stress on brain cells. It may protect nerve cells from damage and improve their function. Research shows that boosting autophagy supports nerve cell survival and slows disease progression.
Hormone Signaling Improvements
Fasting changes hormone levels and their signals in the body. It improves leptin and insulin signaling, hormones that influence brain health and nerve repair. Better hormone signaling helps reduce inflammation and supports brain cell growth.
These hormonal shifts promote nerve regeneration and protect brain cells. They also help maintain energy balance in neurons, which is crucial for people with Parkinson’s. Improved hormone signaling may enhance overall brain function during fasting.
Neuroprotection Benefits
Fasting shows promising neuroprotection benefits for people with Parkinson’s disease. It helps protect brain cells and supports their health. Experts highlight fasting’s role in reducing harmful processes that damage neurons. This can slow down the progression of Parkinson’s symptoms and improve quality of life.
Research suggests fasting influences key factors that cause nerve cell damage. It targets inflammation and oxidative stress, two major contributors to Parkinson’s disease. These effects help maintain brain function and support nerve repair.
Inflammation Reduction
Fasting lowers inflammation in the brain, which is common in Parkinson’s patients. Chronic inflammation damages neurons and worsens symptoms. Therapeutic fasting reduces inflammatory markers and calms immune responses. This protects nerve cells from ongoing harm and supports brain health. Studies show fasting can decrease brain swelling and improve motor function.
Oxidative Stress Control
Oxidative stress occurs when harmful molecules damage brain cells. It plays a key role in Parkinson’s disease progression. Fasting helps control oxidative stress by boosting antioxidants in the body. These antioxidants neutralize harmful molecules and reduce cell damage. By lowering oxidative stress, fasting supports neuron survival and function. This may slow down nerve cell loss in Parkinson’s disease.
Credit: www.mdpi.com
Nerve Repair Mechanisms
Nerve repair is vital in managing Parkinson’s disease symptoms. Damaged nerve cells can slow movement and cause tremors. Therapeutic fasting may support the body’s natural repair processes. Research shows fasting activates several mechanisms that help nerve healing.
Fasting triggers cellular clean-up and regeneration. It also improves hormone signals that aid nerve recovery. These effects combine to protect and restore brain function. Understanding these nerve repair mechanisms clarifies fasting’s potential benefits for Parkinson’s patients.
Neurogenesis Enhancement
Neurogenesis means creating new nerve cells. Fasting stimulates this process in the brain. New neurons help replace damaged ones, improving brain health. Animal studies show intermittent fasting increases neurogenesis in key brain areas. This growth can support better motor control and memory. Boosting neurogenesis may slow Parkinson’s disease progression.
Neuroplasticity Boost
Neuroplasticity allows the brain to adapt and rewire itself. Fasting enhances this flexibility in nerve connections. Stronger neural networks improve communication between brain cells. This leads to better movement coordination and cognitive function. Studies reveal fasting lowers inflammation and oxidative stress, key factors harming plasticity. Improved neuroplasticity helps the brain compensate for Parkinson’s damage.
Research Evidence
Research evidence on fasting and Parkinson’s disease explores how therapeutic fasting might affect the condition. Scientists study this topic to find new ways to protect nerve cells and slow disease progression. Research includes both animal models and human trials. These studies help us understand fasting’s potential benefits and limits for Parkinson’s patients.
Animal Model Findings
Animal studies show promising results for fasting and Parkinson’s disease. Fasting increases autophagy, the body’s way of cleaning damaged cells. This process may help remove toxic proteins linked to Parkinson’s. Fasting also reduces inflammation and oxidative stress in animal brains. These effects protect nerve cells and improve their function. Some studies report better motor skills and slower disease progression in fasted animals. These findings support the idea that fasting could help manage Parkinson’s symptoms.
Human Study Limitations
Human studies on fasting and Parkinson’s disease are fewer and less conclusive. Many trials have small sample sizes or short durations. Some patients find strict fasting hard to follow consistently. Results vary widely due to different fasting methods and patient conditions. More research is needed to confirm fasting’s safety and effectiveness in humans. Scientists must also study long-term effects and optimal fasting schedules. Current evidence suggests potential but does not prove fasting as a treatment for Parkinson’s disease.
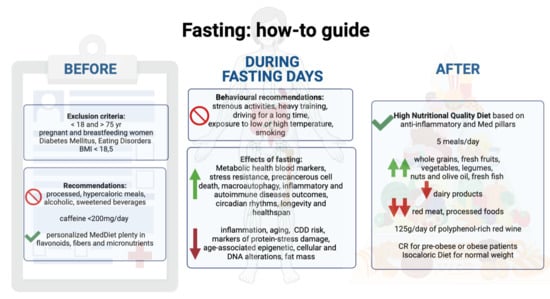
Safety And Precautions
Fasting may offer benefits for Parkinson’s disease, but safety must come first. Understanding precautions helps avoid harm and supports positive outcomes. Careful planning and awareness reduce risks linked to fasting practices.
Medical Consultation Importance
Consult a doctor before starting any fasting routine. Parkinson’s disease affects the brain and body in complex ways. A healthcare professional can assess your health and recommend safe fasting methods. They can adjust medications or suggest alternatives. Regular monitoring ensures fasting does not worsen symptoms or cause complications.
Potential Risks Of Fasting
Fasting can cause low blood sugar, dizziness, or fatigue. These effects may be stronger in people with Parkinson’s. Skipping meals might affect medication absorption and timing. Dehydration is also a concern during fasting periods. Some may experience headaches or weakness. Long fasting without supervision can increase risk of malnutrition. It is important to recognize warning signs and stop fasting if needed.
Credit: www.mdpi.com
Frequently Asked Questions
Is Fasting Good For Parkinson’s Disease?
Fasting may support Parkinson’s by reducing inflammation and promoting nerve cell repair. Research is mostly in animals. Consult a doctor before starting fasting for Parkinson’s management.
What Chemical Is Strongly Linked To Parkinson’s Disease?
The chemical strongly linked to Parkinson’s disease is paraquat, a widely used herbicide. Exposure increases Parkinson’s risk.
Can Autophagy Cure Parkinson’s Disease?
Autophagy may help clear damaged cells linked to Parkinson’s but cannot cure the disease. Research is ongoing.
Can Fasting Repair Nerve Damage?
Fasting may support nerve repair by boosting autophagy, reducing inflammation, and enhancing neuroplasticity. Most evidence comes from animal studies. Human research is limited, so consult a healthcare professional before trying fasting for nerve damage.
Conclusion
Fasting shows promise in supporting nerve health and reducing Parkinson’s symptoms. Experts highlight benefits like reduced inflammation and improved brain cell repair. Most findings come from animal studies, so human research is needed. Therapeutic fasting may complement traditional treatments but should be discussed with a doctor.
It offers hope but is not a cure. Staying informed and cautious helps make better health choices.
